 Health
Health
 Ticks
Ticks
 There are 11 species of tick in the North East US.
There are 11 species of tick in the North East US.
See Tick Species | TickEncounter.org - U. Rhode Island
Tickborne Diseases of the United States at the CDC lists 7 species
Ticks are carriers of lyme disease (LD), Ehrlichiosis, Babesiosis and others.
See A single tick bite could put you at risk for at least 6 different diseases | Business Insider
The CDC lists 17 tick borne diseases.
If a tick is attached to your skin for less than 24 hours, your chance of getting Lyme disease is extremely small.
The states with the highest incidence of Lyme disease (10-80 times the rest of the country) are: Connecticut, Delaware, District of Columbia, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, West Virginia , Wisconsin,
Larval Tick Infestation: A Case Report and Review of Tick-Borne Disease | MDedge Dermatology
Larvae (sometimes referred to as seed ticks) measure from 0.5 to 0.8 mm in diameter and often are difficult to recognize because of their small size.4,5 Nymphs are approximately 1.5 mm in diameter and adults can be 5 mm in diameter. Both the nymphs and adults are 8 legged, while larvae have 6 legs.
The 2-year life cycle of ticks consists of 4 stages: egg, larva, nymph, and adult. Larvae (sometimes referred to as seed ticks) measure from 0.5 to 0.8 mm in diameter and often are difficult to recognize because of their small size.4,5 Nymphs are approximately 1.5 mm in diameter and adults can be 5 mm in diameter. Both the nymphs and adults are 8 legged, while larvae have 6 legs.
Because they are so hard to spot, infected nymphs cause the vast majority of Lyme disease cases in humans. In fact, a significant number of patients diagnosed with Lyme never saw the tick that bit them in the first place.
Removal:
 The Tick Nipper was recommended in "Evaluation of Three Commercial Tick Removal Tools" from Ohio State's Acarology Lab.
The Tick Nipper was recommended in "Evaluation of Three Commercial Tick Removal Tools" from Ohio State's Acarology Lab.
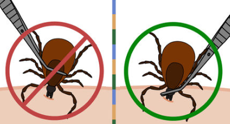 4 ways to remove a tick | wikiHow
4 ways to remove a tick | wikiHow
Use fine-tipped tweezers / Forceps (bent or curved tip are best) to firmly grasp the tick very close to your skin.
 With a steady motion, pull the tick away from your skin. Then clean your skin with soap and warm water.
With a steady motion, pull the tick away from your skin. Then clean your skin with soap and warm water.
This article states:
Timely removal is critical for avoiding tick-transmitted diseases by reducing
the interval for pathogen entrance into the host. Numerous manuals and
textbooks continue to recommend methods for tick removal that are dangerous or simply fail. The most popular methods
are passive and include applying ointments, ether, gasoline or petroleum so
they will release their hold. Others have endorsed applying fingernail polish,
and "using a suture needle (FS-2 cutting) to apply pain to the tick's face for
removal."
Other myths were you had to un-screw the tick and whether it was a right or left handed twist depended on the species.
Needham tested several of these "folk" methods; fingernail polish, petroleum jelly, a glowing hot match and 70% isopropanol for their ability to induce ticks to "back out" or release from the host. He found that none of these methods initiated self detachment in adult lone star or American dog ticks. Confirmation of the failure of these methods was recently published.
Tick
removal (Ohio State's Acarology Lab)
The following guidelines should be followed.

- Avoid handling ticks with uncovered fingers; use tweezers or commercial tools designed for removal. If index finger and thumb must be used, protect them with rubber gloves, plastic or even a paper towel.
- Place the tips of tweezers or edges of other removal devices around the area where the mouthparts enter the skin.
- With steady slow motion, pull the tick away from the skin or slide the removal device along the skin (read the directions for each commercial tool). Do not jerk, crush, squeeze or puncture the tick.
- If you have broken off their mouth parts under your skin, consult your physician immediately.
- After removal, place the tick directly into a sealable container. Disinfect the area around the bite site using standard procedures.
- Keep the tick alive for a month in case symptoms of a tick-borne disease develop. Place it in a labeled (date, patient), sealed bag or vial with a lightly moistened.
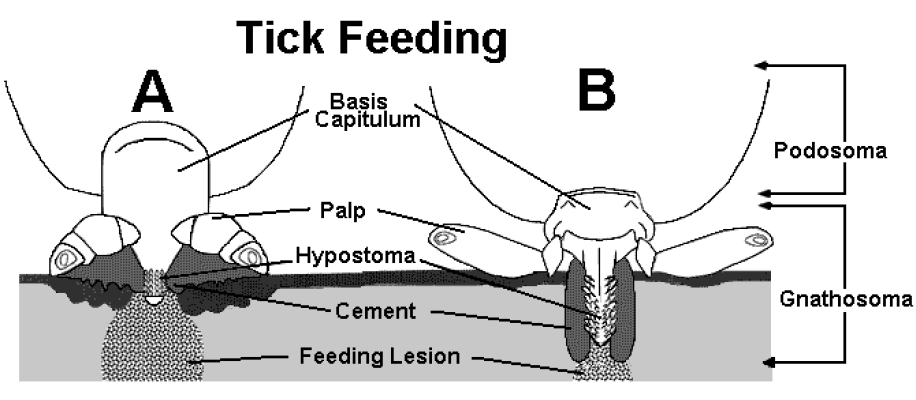
Diagram of tick feeding. Tick A represents a superficial species, such as the American dog tick ( Dermacentor variabilis). Tick B represents a more deeply attached species, such as the lone star tick ( Amblyomma americanum). The leg bearing section is denoted the podosoma while the head region, the gnathosoma. When removal is attempted, the target region for contact with any removal instrument should be between the podosoma and gnathosoma at the basis capitulum.
 Tick Removal (American Lyme Disease Foundation)
Tick Removal (American Lyme Disease Foundation)
Tick's mouthparts have reverse harpoon-like barbs (image at right), designed to penetrate and attach to skin. Ticks secrete a cement-like substance that helps them adhere firmly to the host.
Hundreds of barbs on the outer surface of the hypostome grip the skin like fishhooks as it enters the break in the epithelium. To strengthen its hold, the tick secretes a ring of cement around the cavity, fixing itself in place for a feast. It is while the tick feeds - a meal that can last several days or a week.
The goal is:
- Remove the tick as soon as possible to minimize or interrupt the transfer of infectious material
- prevent the tick from regurgitating infectious material into the patient
- minimize damage or pain to the patient undergoing the procedure.
"The definitive treatise of tick removal has yet to be published, despite the abundance of anecdotal suggestions in the medical literature." Removal Procedure:
- Use fine-point tweezers * to grasp the tick at the place of attachment, as close to the skin as possible. DO NOT grasp the tick by the body.
- Gently pull the tick straight out. DO NOT grasp the tick by the body.
- Place the tick in a small vial labeled with the victim's name, address and the date.
- Wash your hands, disinfect the tweezers and bite site.
- Mark your calendar with the victim's name, place of tick attachment on the body, and general health at the time.
- Call your doctor to determine if treatment is warranted.
- Watch the tick-bite site and your general health for signs or symptoms of a tick-borne illness. Mark any changes in your health status on your calendar.
- If possible, have the tick identified/tested by a lab, your local health department, or veterinarian.
Sources: The Centers for Disease Control and Prevention (CDC), American Lyme Disease Foundation, Pfizer Reasearch
Lyme Disease: (Summary of information at the American Lyme Disease Foundation)
What is Lyme Disease:
Lyme disease (LD) is an infection caused by Borrelia Borrelia burgdorferi, a type of bacterium called a spirochete (pronounced spy-ro-keet) that is carried by deer ticks. LD manifests itself as a multisystem inflammatory disease that affects the skin in its early, localized stage, and spreads to the joints, nervous system and, to a lesser extent, other organ systems in its later, disseminated stages.
See risks below.
The number of reported cases of Lyme Disease had increased dramatically since its initial discovery in Lyme, Connecticut in 1975.
Early treatment is important for full recovery.
You can get a one shot antibiotic right after the bite as a precaution.
Look for symptoms (below) in 1 to 2 weeks (range = 3 to 30 days).
Symptoms:
The first symptom is usually an expanding rash (called erythema migrans, or EM, in medical terms) which is thought to occur in 80% to 90% of all LD cases.
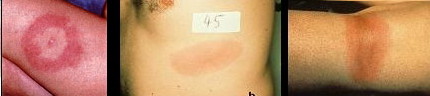
Click for more pictures.
An EM rash generally has the following characteristics:
- Usually (but not always) radiates from the site of the tickbite
- Appears either as a solid red expanding rash or blotch, OR a central spot surrounded by clear skin that is in turn ringed by an expanding red rash (looks like a bull's-eye)
- Appears an average of 1 to 2 weeks (range = 3 to 30 days) after disease transmission
- Has an average diameter of 5 to 6 inches (range = 2 inches to 2 feet)
- Persists for about 3 to 5 weeks
As the LD spirochete (bacteria) continues spreading through the body, a number of other symptoms including severe fatigue, a stiff, aching neck, and peripheral nervous system (PNS) involvement such as tingling or numbness in the extremities or facial palsy (paralysis) can occur.
The more severe, potentially debilitating symptoms of later-stage LD may occur weeks, months, or, in a few cases, years after a tick bite.
Diagnosis:
You can take the tick to a lab for testing:
e.g. New Jersey Laboratories
If the tick is less than 2 weeks old it will cost $65 to test for lyme.
If it is more than 2 weeks or exposed to alcohol or an antibiotic it will require a DNA test $175.
Risks:
Not all ticks are infected, and studies of infected deer ticks have shown that they begin transmitting Lyme disease an average of 36 to 48 hours after attachment.Therefore, your chances of contracting LD are greatly reduced if you remove a tick within the first 48 hours.
Source:
American Lyme Disease Foundation
Estimates are that the prevalence of the spirochete (bacteria) responsible for Lyme disease, in the nymphal stage of the deer tick, in endemic areas of the Northeast and Midwest, is 15% to 30% (The responsible vector in the western states is I pacificus, a deer and cattle tick.) The likelihood of disease transmission from the bite of an infected tick is only 1% to 3%.1
Prevention:
Personal Protection:
Repellents:
Permethrin is best.
Permethrin Fact Sheet | TickEncounter.org - URI
Walmart
Amazon
Typically sprayed on clothing. Will last 3-4 weeks with washings.
Commercially-treated clothes can last up to 70 washings.
It can be sprayed directly on the skin. It is absorbed at 1/20th the rate of DEET.
Terms:
A granuloma is a small area of inflammation (a ball-like collection of immune cells) due to tissue injury. See: Granuloma from Practical Pediatric Dermatology.
Links:
Avoidance | CDC Lyme Disease
Get TickSmart: 10 Things to Know, 5 Things to Do N. Carolina Extension Svc., Dr. Thomas Mather U. Rhode Island
A clinician's guide to safe and effective tick removal at SkyScape.com
American Lyme Disease Foundation
Tick Disease by State
Return to Germs.